Advances in materials, digital workflows, and prosthetic design have transformed what dentures can do for people who have lost teeth. Removable prostheses remain a practical, proven way to restore a complete smile, rebuild chewing function, and support facial contours. While dental implants and fixed bridgework provide important alternatives for many patients, modern dentures offer versatility and predictable outcomes when designed and fabricated with care.
Our approach combines clinical experience with close attention to fit, function, and appearance. Dentures today are crafted from improved acrylics and tooth materials that mimic natural teeth and gums, and they are shaped to harmonize with an individual’s facial features. The goal is not only to replace missing teeth but also to restore confidence and comfort in everyday activities like speaking and eating.
Every denture begins with a careful evaluation of oral health, bone support, and any remaining teeth. From that foundation, we create a plan that balances durability, ease of care, and lifelike aesthetics. Whether you’re losing a few teeth or an entire arch, our team focuses on a prosthesis that feels secure and looks natural.
Losing teeth affects more than appearance. Gaps change how the remaining teeth meet and distribute bite forces, which in time can lead to shifting, uneven wear, and additional tooth loss. When teeth are missing, the jawbone can begin to resorb in the areas no longer stimulated by natural tooth roots, altering facial support and sometimes making future restorations more complex.
Functionally, missing teeth can make it harder to chew a range of foods, which may influence nutrition and digestion. Speech is also affected when front or back teeth are absent, and even small changes in tooth position can alter consonant sounds. For many people, these functional limitations have social and psychological consequences that extend into daily life.
Addressing tooth loss early helps limit progressive changes and preserves more options for long-term care. Whether the solution is a partial denture that fills a few spaces or a complete denture that replaces an entire arch, thoughtful treatment planning aims to restore efficient chewing, clear speech, and a balanced facial appearance.
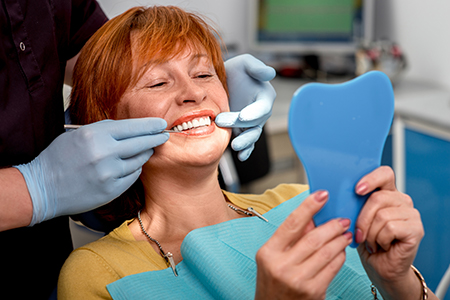
Dentures are removable prosthetic devices that sit on the gums to replace missing teeth. They consist of artificial teeth set into a base that follows the shape of the mouth. Contemporary base materials and artificial teeth are designed to be both durable and lifelike—matching shade, translucency, and tooth form to the patient’s natural dentition and facial features whenever possible.
One of the practical advantages of removable dentures is accessibility: they can be removed for cleaning, allowing better hygiene for the mouth and prosthesis. This removability also makes adjustments and repairs simpler than many fixed options. At the same time, careful design—considering things like border extensions, occlusion, and tissue contact—is essential to achieve comfort and stability during everyday use.
While dental implants and bridges offer fixed restorations for certain cases, dentures remain an important solution when implants or fixed bridgework are not suitable. Dentures can be adapted over time—through relines, repairs, or conversion to implant-supported designs—to meet changing oral health needs.
Choosing the right prosthesis starts with a detailed oral examination and an honest discussion about goals and lifestyle. The primary removable options are full (complete) dentures and partial dentures. The right choice depends on how many natural teeth remain, the health of those teeth, the condition of the gums and bone, and the patient’s functional expectations.
When all teeth in an arch are missing or need to be removed, a full denture is a common solution. In cases where some healthy, stable teeth remain, a partial denture can restore missing teeth while preserving the existing dentition. Partial dentures often use clasps or precision attachments to blend with the remaining teeth and maintain occlusal balance.
We review each patient’s medical and dental history, examine the supporting bone and soft tissues, and consider how the denture will interact with the lips and facial profile. That assessment guides decisions about tooth arrangement, gum contouring on the prosthesis, and whether additional steps—such as extractions or soft tissue adjustments—are advisable before fabrication.
Complete dentures are designed to replace all teeth in the upper or lower arch. Their design varies depending on individual anatomy and expectations. A well-made full denture restores vertical dimension, lip support, and the proper relationship between upper and lower jaws to promote comfortable chewing and a natural appearance.
Some dentures are fabricated after extraction sites have healed, allowing the tissues to settle and the prosthesis to be fitted for a stable, long-term contour. Other approaches provide teeth immediately after extractions to avoid gaps during healing; these immediate dentures are later adjusted or relined as tissues change. Your clinician will explain which timing aligns best with your treatment plan and oral health.
Immediate dentures
Immediate dentures are placed at the time of tooth removal so a patient never has to be without teeth. Because the tissues remodel during healing, these prostheses typically require follow-up adjustments or relines to maintain an optimal fit.
Overdentures
An overdenture receives added support from remaining tooth roots or specially designed implant attachments. This approach preserves bone and improves stability while retaining the benefits of a removable prosthesis.
Implant-supported dentures
Implant-supported designs attach to strategically placed implants, creating a more secure connection between the denture and the jaw. This option is especially useful when retention with tissue support alone is insufficient for function or comfort.
Partial dentures fill one or more spaces when some natural teeth remain. They help restore a complete dental arch, preserve proper spacing, and prevent unwanted drifting of the remaining teeth. Careful design ensures that the prosthesis distributes forces evenly and works in harmony with the existing bite.
Frameworks for partial dentures can be fabricated from metal alloys, flexible resins, or hybrid materials depending on the case requirements and patient preferences. Precision attachments offer a discreet alternative to visible clasps and can improve comfort and appearance.
Good partial denture design aims to preserve tooth and tissue health while making daily wear comfortable. Regular monitoring and maintenance help the appliance continue to perform well as the mouth changes over time.
Our team focuses on long-term fit and function, selecting materials and attachment strategies that suit each patient’s oral condition and lifestyle.

Creating a successful denture is a multi-step process that combines diagnostic imaging, precise impressions, laboratory collaboration, and clinical adjustments. We begin with a comprehensive evaluation that may include digital scans or x-rays to assess bone levels and existing tooth support.
Impressions and bite records allow the dental laboratory to reproduce jaw relationships and design a prosthesis that restores proper occlusion and facial proportions. Teeth are selected for shape and shade that complement the patient’s features, and trial setups give an opportunity to preview how the prosthesis will look and function before final processing.
Once the denture is fabricated, careful insertion and verification of fit are performed. Minor adjustments are common during the initial period of wear as the tissues respond and the patient adapts to the appliance. Our emphasis is on proactive follow-up to resolve sore spots, refine occlusion, and ensure comfortable function.
In some cases, preparatory procedures—such as smoothing sharp bone edges or extracting nonrestorable teeth—are recommended to optimize the fit and longevity of the final denture. We coordinate these steps to reduce surprises and promote a successful transition to the prosthesis.

Adapting to a new denture takes a little time and patience. Initially, speech and chewing may feel different as the lips, tongue, and cheeks learn to work with the prosthesis. Gradual practice—reading aloud, eating soft foods, and cutting food into smaller pieces—helps speed the adjustment period.
Getting comfortable with wear
Minor sore spots are common as the denture settles. Returning for timely adjustments is the best way to resolve irritation and improve fit. Wearing the denture as advised between visits gives the clinician useful feedback about how the appliance performs during real-world use.
Temporary increase in saliva
A temporary increase in saliva production is a normal response when a new appliance is introduced. This typically diminishes as the mouth adapts.
Speech and chewing practice
With time and practice, most people regain clear speech and effective chewing. Simple exercises—such as repeating certain sounds and gradually introducing more challenging foods—help rebuild comfort and confidence.
Denture hygiene and overnight care
Clean dentures daily by rinsing after meals and brushing with a soft brush made for prostheses to remove debris and plaque. Gentle cleaning products formulated for dentures help prevent staining and bacterial buildup.
Continue to care for any remaining teeth and the gums—brushing and cleaning around abutment teeth is essential to preserve oral health and the integrity of the prosthesis.
When not in use, store dentures in water or a recommended soaking solution to prevent drying and distortion. Avoid hot water, which can warp acrylic bases.
Improving stability when needed
Some dentures benefit from supplemental retention, whether through adhesives, attachments, or implant support. When stability is a concern, we discuss options to enhance comfort and function while preserving tissue health.
Regular follow-up and relines
As oral tissues change over months and years, relines or adjustments help restore a snug fit. Routine checkups let us examine soft tissues, evaluate any remaining teeth, and keep your prosthesis performing well.
Our team is committed to helping patients transition to and live well with their dentures. If you’d like to learn more about denture options or discuss how a prosthesis could fit into a broader restorative plan, please contact Dentistry of Sugar Land for additional information.

Today, it’s easier than ever to replace missing teeth and achieve natural-looking, durable, and long-lasting results! Depending on a patient’s dental needs, lifestyle, expectations of care, and budget, choices can include conventional fixed bridgework, dental implants, or removable partial and complete dentures. At the office of Dentistry of Sugar Land, we’ll discuss all your options in care and answer all your questions as you choose the solution that’s right for you.
With advances in dental materials and technology, today’s dentures are more comfortable and realistic-looking than ever before.
Whether you wear partial or complete dentures, it’s essential to see the dentist for routine care. Besides checking the fit and condition of your dentures and making any necessary adjustments, you’ll also receive a comprehensive exam to check on the health of any remaining teeth as well as the soft and hard tissues in and around the oral cavity.
A same-day denture offers an accelerated design and fabrication process that allows a patient to go from impression taking to denture insertion in a single day.
For patients who don’t want to wait after having teeth extracted, an immediate denture can be inserted the same day your teeth are removed. Sometime later you may need the denture relined to address any changes in its fit once the extraction sites have completely healed.
While no one wants to drop or break a partial or complete denture, accidents do happen. The good news is that in some cases, your partial or complete denture is reparable. It all depends on the extent of the damage. Don’t hesitate to contact our office if you’ve broken or damaged your denture. We’re happy to help.
The simple act of taking your partial denture in and out can cause certain types of metal clasps to loosen over time. When you come in for your checkup visit or contact our office for an adjustment, we’ll assess the fit of your partial and tighten the clasps for improved stability and comfort.
While rebuilding a complete smile is a worthwhile investment, our office is sensitive to the costs involved in dental care. We customize care and will discuss which treatment options address your needs, lifestyle, and budget. How much a new denture will cost depends on the type of the prosthesis, its design, and the materials used to fabricate the supportive base, teeth, and clasps or precision attachments. Dentures that include the placement of dental implants for added retention and stability typically involve additional costs.
If you have dental insurance, your coverage may include a new or replacement set of dentures. Our staff is happy to review your coverage with you to ensure you are maximizing your insurance benefits while minimizing any out of pocket expenses.
At the office of Dentistry of Sugar Land, we provide an extensive range of dental services, including the latest and most effective methods to help patients with missing teeth rebuild complete and beautiful smiles. As skilled and experienced professionals, we recognize that every patient is different, and every smile is unique. We’re passionate about what we do and take great pride in providing personalized treatment plans while treating our patients as valued partners in care.
Modern dentures are removable prosthetic appliances that replace missing teeth and their supporting structures, using improved base materials and lifelike tooth resins to better mimic natural dentition. Contemporary designs take advantage of digital workflows and refined prosthetic concepts to improve fit, esthetics, and durability compared with older acrylic-only appliances. Advancements in shade matching, tooth form, and base contouring allow technicians to create prostheses that harmonize with facial features and speech patterns.
Today's dentures also prioritize functional factors such as occlusion, border extensions, and tissue contact to enhance chewing efficiency and stability. Many designs can be adjusted, relined, or converted to implant-supported options as oral conditions change over time. Because they are removable, modern dentures provide accessibility for cleaning and relatively straightforward repairs when needed.
Candidates for dentures include people who are missing multiple teeth or an entire dental arch, those whose remaining teeth are not restorable, and patients whose bone or medical conditions make fixed solutions impractical. A thorough clinical evaluation of oral health, bone support, gum condition, and medical history helps determine whether a removable prosthesis is appropriate. Functional expectations, lifestyle, and the patient’s willingness to follow maintenance recommendations are also important factors in candidacy.
In some cases, patients who are otherwise suitable for implants may still choose dentures for reasons such as treatment timeline, surgical considerations, or personal preference. Partial dentures are indicated when some healthy teeth remain and can be used to preserve spacing and prevent drifting. The treatment plan is individualized to balance comfort, esthetics, and long-term oral health.
Full dentures, also called complete dentures, replace all teeth in either the upper or lower arch and rely primarily on tissue support and proper border seal for retention. They are designed to restore vertical dimension, lip support, and occlusal relationships to promote comfortable chewing and a natural appearance. Partial dentures replace one or more missing teeth when healthy natural teeth remain and typically use clasps, precision attachments, or a supporting framework to integrate with the existing dentition.
Partial frameworks can be made from metal alloys, flexible resins, or hybrid materials depending on clinical needs and patient preference, and they are intended to distribute forces evenly to preserve remaining teeth. Full and partial designs are selected based on the number and condition of remaining teeth, bone volume, and the overall restorative plan. Proper design and regular monitoring help maintain occlusal stability and tissue health over time.
Immediate dentures are placed at the time of extractions so the patient does not go without teeth during the healing period, but they typically require relines or adjustments as tissues remodel. Immediate appliances can help preserve esthetics and function during recovery, though follow-up care is essential to maintain fit and comfort. Clinicians will plan for interim adjustments and eventual definitive prostheses when healing is complete.
Overdentures gain additional support from retained tooth roots or attachments to help preserve bone and improve stability, while implant-supported dentures attach to dental implants for enhanced retention and chewing ability. Implant-supported designs range from removable overdentures on locators or bars to fixed hybrid prostheses, depending on patient needs and bone availability. These options allow clinicians to tailor retention and maintenance strategies as part of a long-term restorative plan.
Planning begins with a comprehensive examination that may include digital scans or radiographs to assess bone levels, remaining teeth, and soft tissue anatomy. Precise impressions, bite records, and careful tooth selection are used to reproduce jaw relationships and design a prosthesis that supports correct occlusion and facial proportions. Laboratory collaboration and trial setups allow patients and clinicians to evaluate esthetics and function before final processing.
After fabrication, insertion involves verification of fit, occlusion, and phonetics, with minor adjustments commonly needed as the patient adapts and tissues settle. Preparatory procedures such as smoothing sharp bone edges or removing nonrestorable teeth may be coordinated to optimize outcomes. The process emphasizes proactive follow-up to address sore spots, refine occlusion, and ensure the prosthesis performs well in daily use at Dentistry of Sugar Land.
Adapting to new dentures often involves an initial period of altered speech, increased saliva production, and sensitivity as the lips, tongue, and cheeks learn new movements around the appliance. Minor sore spots are common and generally respond quickly to timely adjustments by the dental team. Patients are usually advised to start with soft foods, cut items into smaller pieces, and practice speaking aloud to accelerate adaptation.
Regular short follow-up visits during the first weeks allow clinicians to refine fit and occlusion and to address any areas of irritation. Wearing the denture as instructed between visits helps the clinician observe real-world performance and make informed adjustments. Over time, most patients regain efficient chewing and clear speech as comfort improves and the tissues accommodate the prosthesis.
Daily hygiene for dentures includes rinsing after meals, brushing with a soft brush designed for prostheses, and using gentle, denture-specific cleaners to remove debris and biofilm. It is important to avoid abrasive household cleaners and hot water that can warp acrylic bases, and to clean any remaining natural teeth and gums thoroughly to protect oral health. Storing dentures overnight in water or a recommended soaking solution helps prevent drying and distortion of the base.
Routine inspection of the appliance for cracks, worn teeth, or loose components helps identify issues early so repairs can be made before problems worsen. If adhesives are used, follow manufacturer instructions and discuss long-term strategies with your clinician to avoid masking fit problems. Consistent daily care combined with periodic professional evaluation preserves function and appearance over time.
Stability and retention can be enhanced by optimizing denture design elements such as border extensions, occlusal schemes, and tissue contact, all of which are planned during fabrication. Additional retention can be achieved with adhesives, precision attachments, or converting a removable prosthesis to an implant-supported design when clinical conditions allow. Overdentures that use remaining roots or implant attachments help preserve bone and provide greater confidence during chewing and speaking.
When retention is a concern, a clinician will evaluate bone volume, muscle dynamics, and existing prosthesis design to recommend the least invasive and most predictable solution. Sometimes a reline or adjustment will restore adequate fit, while other times supplemental support through implants or attachments offers a longer-term improvement. The chosen approach always seeks to balance comfort, oral health, and the patient’s functional needs.
Dentures should be evaluated at regular dental checkups to monitor fit, tissue health, occlusion, and the condition of any remaining teeth or implants. Routine examinations allow the clinician to detect changes in oral tissues that may necessitate a reline, repair, or adjustment to maintain comfort and function. Relines are commonly recommended when the denture no longer fits snugly due to tissue remodeling or gradual bone changes.
A reline restores a close fit between the denture base and the tissues and can often extend the useful life of a prosthesis when done appropriately. If persistent instability, sore spots, or wear are present, the provider will discuss whether a reline, repair, or a new prosthesis is the best option. Scheduling periodic follow-up helps prevent complications and ensures the appliance continues to meet functional needs at Dentistry of Sugar Land.
Well-designed dentures restore chewing function and enable a broader diet than would be possible with missing teeth, improving the ability to process foods that support good nutrition. Initially, patients may need to modify eating habits and progress from soft to firmer foods as they regain confidence and chewing coordination. Proper tooth arrangement and vertical dimension also influence speech by supporting correct tongue and lip positioning for clear consonant production.
By replacing lost tooth structure and supporting soft tissues, dentures help preserve facial contours and reduce the appearance of collapse that can accompany advanced tooth loss. Thoughtful prosthetic design addresses lip support and lower facial height to create a balanced profile and a natural-looking smile. Ongoing maintenance and timely adjustments are important to sustain these functional and esthetic benefits over time.
Ready to schedule your next dental appointment or have questions about our services?
Contacting Dentistry of Sugar Land is easy! Our friendly staff is available to assist you with scheduling appointments, answering inquiries about treatment options, and addressing any concerns you may have. Whether you prefer to give us a call, send us an email, or fill out our convenient online contact form, we're here to help. Don't wait to take the first step towards achieving the smile of your dreams – reach out to us today and discover the difference personalized dental care can make.