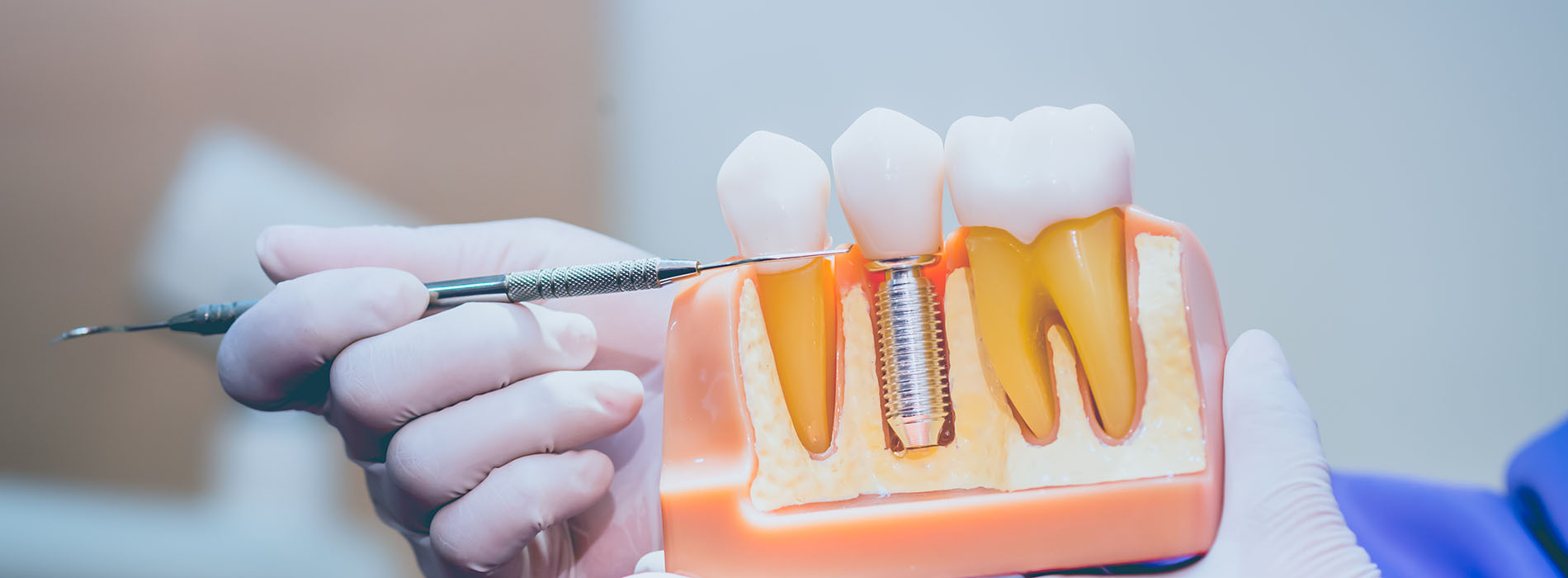
Implant restorations are the visible, functional replacement teeth attached to dental implants — the small, biocompatible posts surgically placed into the jaw to act like natural tooth roots. While implants themselves provide the foundational support, restorations are the customized crowns, bridges, or dentures that restore chewing ability, speech, and the appearance of your smile. In short, restorations turn an implant from a medical anchor into a comfortable, attractive tooth you can use every day.
Many patients appreciate that implant restorations are designed to integrate with the rest of the mouth. Rather than relying on adjacent teeth for support, an implant restoration stands on its own, which helps preserve nearby tooth structure and maintain overall oral integrity. Modern materials and fabrication techniques also allow restorations to match neighboring teeth in color, translucency, and shape so the result looks natural and balanced.
Because these restorations are intended to be long-lasting, they are crafted with both strength and esthetics in mind. The result should feel stable during everyday activities — eating, speaking, and smiling — while blending in cosmetically. A restoration placed with thoughtful planning and precision can provide many years of service with the right care and maintenance.
The process begins with careful evaluation and planning. Your clinician will review medical and dental history, take diagnostic images, and assess bone volume and gum tissue to determine the ideal implant placement. Detailed planning ensures the restoration will not only fit well but also align with bite forces and facial proportions. In some cases, preparatory procedures such as bone grafting or soft-tissue management are recommended to create the right foundation.
Once the implant is placed, there is an integration phase during which the bone bonds to the implant surface — a process that provides a stable base for the restoration. This healing interval varies by situation, but it is a critical step that supports long-term success. During healing, temporary prosthetics can often be provided so patients regain form and function while the underlying implant matures.
After integration, the restorative phase begins. Impressions or digital scans capture the exact shape of your mouth, which allows the dental laboratory to craft a restoration tailored to your anatomy and aesthetic preferences. Your clinician will check fit, color, and occlusion (bite) and make any necessary adjustments before permanently attaching the restoration. The final step is verification of comfort and function — a properly executed restoration should feel natural and require only routine maintenance.
Occasionally, clinicians use coordinated techniques such as custom abutments or screw-retained designs to improve access for hygiene or to achieve specific esthetic effects. These decisions are made case by case to match clinical needs and patient goals, always prioritizing long-term health and predictable results.
Implant restorations are not one-size-fits-all. A single missing tooth is commonly restored with a single crown attached to an implant, while several adjacent missing teeth may be restored with an implant-supported bridge. For patients missing most or all teeth, implant-retained overdentures or full-arch fixed restorations provide stability and improved function compared with traditional removable dentures. Each option is selected according to the number of missing teeth, bone support, and patient preferences.
Material choices play a major role in how a restoration looks and performs. Ceramic materials such as zirconia and high-quality porcelain offer excellent esthetics and biocompatibility, making them strong choices for front and back teeth alike. Metal-ceramic combinations are still used in situations that require extra strength. Your clinician will recommend the most appropriate material based on occlusal demands, esthetic goals, and long-term considerations.
Design options also affect maintenance and reparability. Screw-retained restorations allow easier access for repairs or removal without affecting the crown, while cement-retained restorations may provide a more seamless emergence profile in some esthetic zones. Discussing these nuances with your clinician helps ensure the chosen restoration balances appearance, hygiene access, and serviceability.
With diligent home care and regular professional checkups, implant restorations are known for their durability. Daily brushing and flossing around the restoration — and, when recommended, using interdental brushes or water flossers — help maintain healthy tissues and prevent complications. Routine evaluations let the dental team monitor occlusion and wear, polish restorations as needed, and address any emerging concerns early on.
It’s important to recognize that while the implant post itself is resistant to decay, the surrounding gum tissue can develop inflammation if not cared for properly. Peri-implant mucositis and, in more advanced cases, peri-implantitis are preventable with consistent hygiene and timely professional care. Regular cleanings and periodontal assessments are an integral part of a long-term maintenance plan to preserve both the restoration and the supporting bone.
Minor adjustments or repairs are sometimes required over time — for example, replacing a worn crown or addressing a loosened screw — but these interventions are typically straightforward when detected early. A proactive approach to maintenance helps protect your investment and keeps the appearance and function of the restoration predictable for years to come.
Successful implant restorations depend on coordinated care, combining surgical expertise, restorative skill, and laboratory craftsmanship. At Dentistry of Sugar Land, treatment planning emphasizes communication between the clinician and dental technician so restorations are made to fit both the mouth and the patient’s smile goals. Precision in planning and a methodical approach to each phase of care reduces surprises and improves outcomes.
When you consult with our team, you can expect a thoughtful evaluation that reviews available options and explains the clinical reasoning behind recommendations. We prioritize conservative decision-making that preserves natural tissue whenever possible and tailor restorative choices to each patient’s function and esthetic priorities. Clear expectations and transparent discussion help patients feel informed and confident about their care plan.
During the restorative phase, attention to detail guides every step: accurate impressions or scans, careful shade selection, and trial fittings to refine contours and contacts. Post-restoration, we provide personalized hygiene guidance and a follow-up schedule to safeguard long-term success. Our approach is designed to deliver implant restorations that look natural, perform reliably, and integrate comfortably into daily life.
In summary, implant restorations combine modern materials, thoughtful design, and coordinated clinical care to recreate the look and function of natural teeth. If you would like to learn more about how implant restorations could restore your smile and oral function, please contact us for more information.
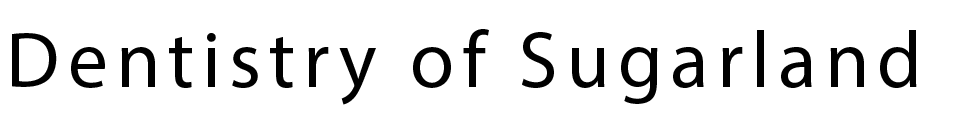
Implant restorations are the visible prosthetic teeth attached to dental implants, while implants are the titanium or zirconia posts surgically placed into the jaw that act like tooth roots. The restoration can be a crown, bridge, or denture and is designed to restore chewing, speech, and the appearance of a natural tooth. Together, the implant and restoration recreate the function and look of a lost tooth in a way that does not rely on neighboring teeth for support.
Restorations are custom-made to match adjacent teeth in size, shape, and color so they blend naturally with your smile. Modern restorative materials and laboratory techniques allow for precise color matching and anatomical contours, improving both esthetics and comfort. Proper design and placement also aim to distribute bite forces evenly to protect surrounding structures and ensure long-term function.
Good candidates typically are adults who are missing one or more teeth and have adequate jawbone volume or are willing to undergo preparatory procedures to develop a stable foundation. A thorough clinical examination, diagnostic imaging, and review of medical and dental history help determine whether an implant restoration is appropriate. Healthy gum tissue and good overall health support successful outcomes, and many common medical conditions can be managed in coordination with a physician.
Patients who smoke or have uncontrolled systemic conditions such as poorly managed diabetes may receive recommendations to optimize health before proceeding, because these factors can influence healing. In some cases, bone grafting or soft-tissue procedures are suggested to improve long-term stability and esthetics. Your clinician will outline individualized options and preparatory steps so you understand the path to a predictable restoration.
The process begins with a comprehensive evaluation that includes diagnostic imaging and treatment planning to determine optimal implant position and restorative design. If necessary, preparatory treatments like tooth extraction, bone grafting, or gum procedures are completed to create the right foundation for long-term success. Once the site is ready, the implant post is surgically placed and allowed to integrate with the bone during a healing phase.
After osseointegration, impressions or digital scans capture precise details for the laboratory to fabricate the restoration. A provisional restoration may be used during this phase to maintain form and function while the final crown, bridge, or denture is produced. At the final appointment the clinician verifies fit, color, and bite before attaching the restoration, then provides care instructions and a maintenance schedule.
Options include single crowns for individual missing teeth, implant-supported bridges for several adjacent missing teeth, and implant-retained dentures or fixed full-arch restorations for patients missing most or all teeth. The choice depends on the number of missing teeth, the quality and quantity of available bone, esthetic goals, and the patient's preferences for removability versus a fixed solution. Each design offers different advantages in terms of stability, hygiene access, and reparability.
Clinicians also consider whether a restoration will be screw-retained or cement-retained, as each approach affects maintenance and emergence profile. Screw-retained designs can simplify retrieval for repairs, while cement-retained options sometimes provide a smoother appearance in certain esthetic zones. A careful discussion about daily care and clinical priorities helps determine the best restoration type for each patient.
Common materials include all-ceramic options such as zirconia and high-quality porcelain, as well as metal-ceramic combinations for cases requiring extra strength. Zirconia offers excellent strength and a toothlike translucency that suits both front and back teeth, while porcelain fused to metal remains a reliable choice when maximum load-bearing capacity is needed. Material selection balances esthetic goals with functional demands to produce a durable, natural-looking result.
Custom abutments made from titanium or zirconia are often used to optimize the emergence profile and soft-tissue support around the restoration. Laboratory craftsmanship and accurate shade communication ensure the final restoration matches surrounding dentition in color and surface texture. Your clinician will recommend materials that address your bite forces, smile expectations, and long-term maintenance needs.
Implant restorations are designed for long-term function when supported by good oral hygiene, routine professional care, and periodic evaluations to monitor wear and occlusion. Daily brushing and flossing around the restoration, supplemented with interdental brushes or water flossers when appropriate, help maintain healthy peri-implant tissues. At Dentistry of Sugar Land we emphasize a preventive schedule of cleanings and examinations so issues can be identified and managed early.
Minor interventions such as replacing a worn crown or tightening a loose screw are uncommon but straightforward when detected promptly. Regular professional assessments also allow clinicians to check bite relationships and polish restorations to reduce surface wear. Staying proactive with home care and follow-up appointments protects both the restoration and the supporting bone over time.
Like any dental procedure, implant restorations carry potential risks such as infection, soft-tissue inflammation, or implant failure in rare cases. Peri-implant mucositis, an inflammation of the soft tissues, can progress to peri-implantitis if not treated, which may affect the supporting bone. Surgical risks such as nerve irritation or sinus involvement are uncommon and are minimized through careful planning and imaging.
Many complications are preventable or manageable with early detection, proper hygiene, and routine professional care. Lifestyle factors and systemic health can influence risk, so clinicians work with patients to modify controllable factors and coordinate care when medical conditions are present. Transparent communication about potential risks and expected outcomes supports safer, more predictable treatment.
Effective home care includes brushing twice daily with a soft-bristled brush and cleaning around the restoration using floss, interdental brushes, or a water flosser as recommended by your clinician. Gentle technique around the gumline helps preserve soft tissues while removing plaque that could contribute to inflammation. Using nonabrasive toothpaste and avoiding hard impacts on the restoration reduce the chance of surface damage.
In addition to daily care, follow any personalized instructions your provider gives about cleaning under and around prosthetic components, especially for implant-retained dentures or bridges. Report any sensitivity, looseness, or persistent swelling to your dental team promptly so issues can be evaluated. Combining diligent home care with scheduled professional visits offers the best protection for long-term success.
Implant restorations help preserve surrounding teeth by replacing missing teeth without relying on adjacent natural teeth for support, which reduces the need to alter healthy tooth structure. Implants stimulate the jawbone and help prevent the bone loss that typically follows tooth loss, supporting facial structure and long-term oral health. Because implants act independently, they can stabilize occlusion and prevent shifting of neighboring teeth into empty spaces.
Successful preservation of bone often depends on timely intervention and, when necessary, supplemental procedures such as bone grafting to rebuild deficient areas. Proper prosthetic design and occlusal planning distribute bite forces to protect both the implant and natural teeth. Regular monitoring ensures that bone levels and the health of surrounding tissues remain stable over time.
Select a team that demonstrates coordinated care, clear communication, and appropriate training in both the surgical and restorative phases of implant treatment. Look for clinicians who use diagnostic tools such as CBCT imaging and digital impressions to plan precise implant placement and restorations, and who involve the dental laboratory early in treatment planning. A practice that explains options, the rationale behind recommendations, and a realistic timeline helps set clear expectations.
Consider a local practice with a track record of collaborative care and thorough follow-up, since long-term maintenance is a critical part of implant success. Dentistry of Sugar Land provides comprehensive planning and patient education tailored to individual needs and esthetic goals in the Sugar Land community. Choosing a team that prioritizes ongoing monitoring and hygiene support improves predictability and patient confidence throughout the restorative journey.
Ready to schedule your next dental appointment or have questions about our services?
Contacting Dentistry of Sugar Land is easy! Our friendly staff is available to assist you with scheduling appointments, answering inquiries about treatment options, and addressing any concerns you may have. Whether you prefer to give us a call, send us an email, or fill out our convenient online contact form, we're here to help. Don't wait to take the first step towards achieving the smile of your dreams – reach out to us today and discover the difference personalized dental care can make.