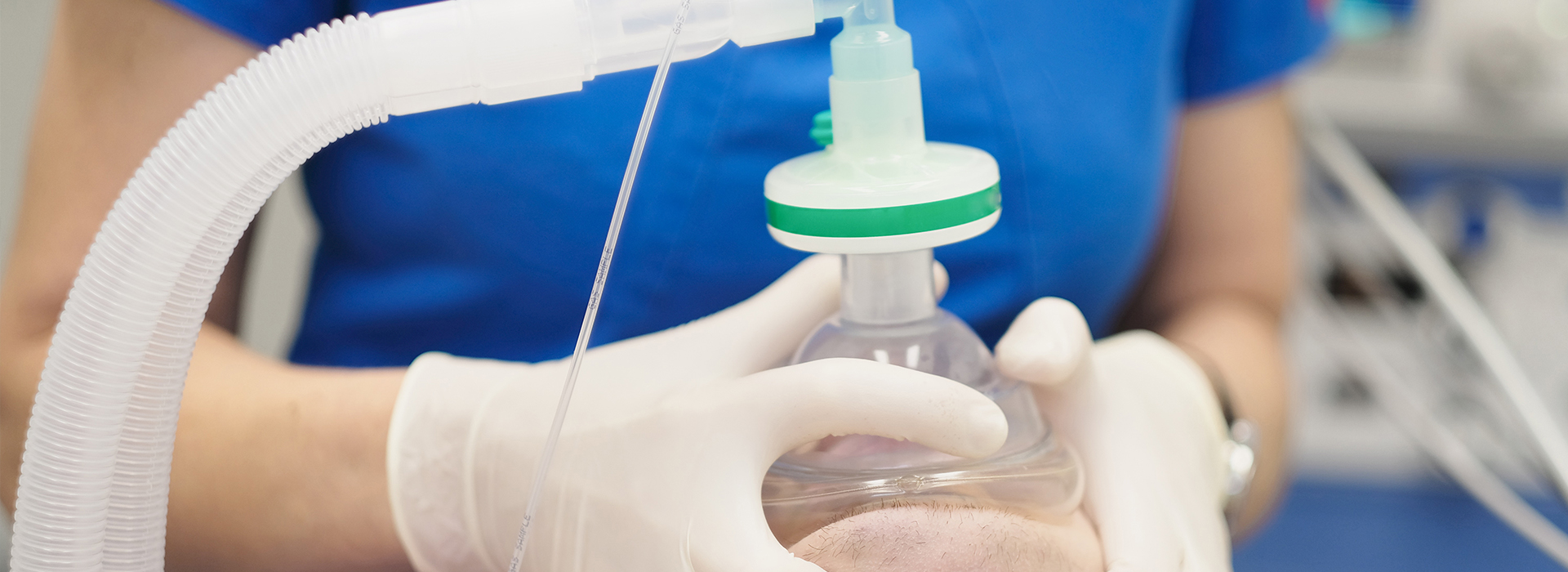
Dental anxiety affects millions of people across the United States, and it’s a common reason patients delay or avoid needed care. If the thought of a dental visit makes you tense, Dentistry of Sugar Land offers respectful, evidence-based sedation options designed to ease fear and help you get the treatment you need. Our approach focuses on safety, comfort, and clear communication so you feel supported at every step.
Avoiding the dentist because of anxiety can allow small problems to grow into more complex issues. Sedation dentistry creates a calmer, more manageable experience so patients can complete necessary procedures with less stress. By pairing sedation with standard local anesthesia and careful monitoring, we help patients leave the office with their oral health restored and their anxiety reduced.
We tailor sedation to each person's needs rather than taking a one-size-fits-all approach. During an initial consultation, our team reviews your medical history, discusses your comfort goals, and explains the options so you can make an informed choice. The result is a plan that balances effectiveness with safety and dignity.
Sedation dentistry is not about putting patients to sleep; it’s about reducing the emotional and physical barriers that make dental care difficult. Depending on the method chosen, sedation can lessen fear, blunt unpleasant sensations, and shrink the perception of time — making even lengthy visits feel more tolerable. Many patients describe the experience as calm and manageable rather than frightening.
Most sedation techniques are used alongside local anesthetic so the procedure itself is pain-free. The sedative medications target the brain’s anxiety pathways to produce a relaxed state while preserving breathing and other vital functions under professional supervision. This combination allows our clinicians to work efficiently and safely while the patient remains comfortable.
Importantly, conscious forms of sedation keep patients able to follow simple verbal cues, which adds a layer of safety and communication throughout the procedure. For those who require deeper levels of sedation, additional safeguards and monitoring are used so that patient wellbeing remains the primary focus from start to finish.
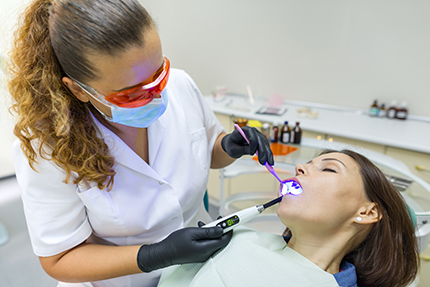
Sedation is a helpful option for a wide range of patients. People with long-standing dental fear often find that sedation makes routine care—cleanings, fillings, and exams—possible and even straightforward. When anxiety gets in the way of preventive visits, sedation can break the cycle of avoidance so oral problems are treated early.
Patients facing complex or lengthy procedures also benefit: sedation helps them remain comfortable and reduces the fatigue that comes from holding the mouth open for extended periods. Additionally, sedation is useful for anyone with a sensitive gag reflex, strong tooth sensitivity, or medical conditions that make sitting still difficult.
Children with severe behavioral challenges and adults with certain cognitive or physical limitations may be candidates for specific sedation approaches when standard techniques are insufficient. Every potential candidate is evaluated carefully — the decision to use sedation always follows a thoughtful review of risks, benefits, and alternative strategies.
Dental phobia or high anxiety — For individuals who feel paralyzed by fear, sedation opens the door to treatment without trauma.
Anticipation of a long or complex procedure — Sedation improves comfort during multi-hour appointments and makes combining treatments possible when medically appropriate.
Pronounced gag reflex or oral sensitivity — Sedation can blunt reflexes and sensory responses so clinicians can work effectively.
Physical or cognitive limitations — When staying motionless for care is a challenge, sedation enables safe, controlled treatment.
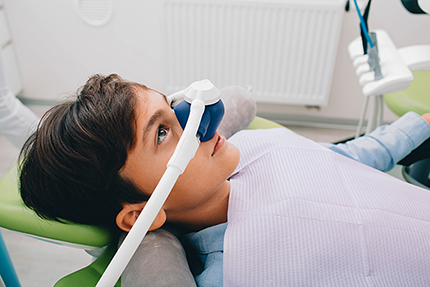
Our practice offers several forms of conscious sedation that are suitable for use in a dental office setting. The right choice depends on your health history, the type and length of the procedure, and your personal comfort goals. All methods are administered by trained clinicians and accompanied by appropriate monitoring.
Before recommending a technique, we review medications you take, any medical conditions, and previous experiences with anesthesia. That background helps us select an approach that provides reliable relaxation while minimizing risk. We emphasize transparency so you know what to expect before you arrive.
Conscious sedation keeps patients in a relaxed, semi-awake state where they can respond to simple commands and breathe independently. This level of sedation is sufficient for the majority of dental procedures performed in an office setting and allows for quicker recovery than general anesthesia.
General anesthesia produces a deeper, fully unconscious state and is reserved for situations where office-based sedation is not appropriate. It requires administration and monitoring in a hospital or surgical center by an anesthesiologist. Our team will recommend that level of care only when it is clearly necessary for medical or safety reasons.
Conscious sedation comes in several forms. Each has advantages and considerations, so we discuss the expected effects and any required preparations before your appointment. Below are the common options you may encounter.
Nitrous oxide, often called “laughing gas,” is a mild sedative delivered through a small nasal mask. It eases anxiety quickly and is easily controlled during treatment. Effects wear off within minutes after the gas is stopped, allowing most patients to leave the office without an escort once they feel alert and steady.
This method is ideal for patients with mild to moderate anxiety and those who want a short-acting, reversible option. Because the level of sedation is adjustable, clinicians can tailor the experience as treatment progresses.
Oral sedation involves taking a prescribed medication before your visit to produce a deeper sense of calm. The dose is selected to match the level of anxiety and the complexity of the procedure. Patients typically feel drowsy and very relaxed; some may have limited memory of the appointment.
Because oral sedatives can impair coordination and judgment for several hours, patients must arrange for a responsible adult to accompany them to and from the appointment. We provide clear pre-visit instructions to maximize safety.
IV sedation delivers medication directly into the bloodstream for rapid and controllable effects. It is used when a deeper, sustained level of sedation is required. One advantage is that the clinician can adjust the medication quickly to maintain the desired comfort level throughout a longer procedure.
IV sedation requires specific pre-appointment preparation, including fasting for a prescribed period beforehand. Patients receiving IV sedation must have a responsible escort available to drive them home and remain attentive after the visit until the effects have fully diminished.
Safety starts before you arrive. For some types of sedation you will be asked to fast for a number of hours, temporarily stop certain medications, and confirm a list of current prescriptions and medical conditions. We’ll provide a clear checklist tailored to the sedation method chosen so you know exactly how to prepare.
On the day of treatment, you can expect monitoring equipment to be in place and a focused review of your health status. Our team will explain how we will watch vital signs and maintain airway and cardiovascular stability. Communication remains open throughout the procedure so you always know what is happening.
After sedation, recovery times vary by method. Nitrous oxide wears off quickly; oral and IV sedatives require more time for the effects to dissipate. Patients are advised to rest for the remainder of the day, avoid driving or heavy machinery, and follow any written aftercare instructions we provide. If you experience unexpected symptoms, we instruct you on when to contact the office or seek immediate care.
Choosing sedation is a collaborative decision. During your consultation we’ll review the benefits and limitations of each option, address your questions, and develop a personalized plan that aligns with your comfort, medical profile, and treatment needs. Our goal is to make the process as clear and reassuring as possible.
Our team is experienced in delivering office-based sedation with the appropriate training and monitoring tools. Whether your priority is easing fear, completing complex restorative work in fewer visits, or simply having a calmer experience, we aim to provide compassionate care grounded in best practices.
To learn whether sedation dentistry is right for you, contact us for more information. We’re happy to explain the options and schedule a consultation to review your needs and preferences.
Sedation dentistry offers patients with general anxiety or fears about a dental procedure the opportunity to have a more comfortable and stress-free experience. By utilizing safe and controlled sedation techniques, the patient is eased into a state of complete relaxation before the procedure. This approach eliminates discomfort, pain, and preoperative anxiety, and typically makes patients feel more at ease post-operatively, as they have little or no memory of the actual moment-to-moment procedure.
Local anesthesia involves an injection directly into or close to the area where a procedure is being performed. While it eliminates any sensation of pain in the targeted area, it does not affect your state of mind or level of anxiety. When a patient receives sedation, additional medications to ease anxiety and promote relaxation are employed in advance of local anesthesia. In this way, both the stress and discomfort associated with a procedure are eliminated. Sedation can be administered in a variety of forms based upon patient needs and the recommendations of the dentist or dental anesthesiologist.
Choosing the most appropriate method of sedation for a procedure depends on a variety of factors such as a patient's medical history and their level of anxiety. Dental sedation can come in the form of nitrous oxide sedation, oral conscious sedation, and IV sedation. Certain patients receiving comprehensive treatment or undergoing a complex surgical procedure may require general anesthesia in a hospital setting.
Nitrous oxide, or "laughing gas," is a mild sedative, which is inhaled through a small mask over the nose. A standard in dental sedation for decades, the effects of nitrous oxide are almost immediate and wear off quickly once your procedure is completed.
Oral sedation involves the prescription of an oral medication prior to your appointment. Taken at the recommended time before your visit, oral sedation allows you to feel fully relaxed by the time you're ready for your procedure. With oral sedation, it's necessary to plan on having an escort to and from your dentist's office.
IV Sedation is administered intravenously, or directly into a vein. It is typically indicated when a deeper state of sedation is required. Your dentist will provide you with specific instructions before your visit, and require that you have an escort for the trip home from your appointment.
Sedation dentistry uses medication to reduce anxiety and increase comfort during dental care. It ranges from mild relaxation with nitrous oxide to deeper, controlled sedation with oral or intravenous medicines. Sedation is typically paired with local anesthesia so the procedure itself is pain-free and more tolerable for the patient.
The goal is to create a calm, cooperative experience that allows clinicians to complete necessary treatment safely and efficiently. Sedation does not always mean being fully unconscious; many office-based techniques keep patients in a semi-awake, responsive state. Treatment plans are individualized so each patient receives the level of sedation that best matches their medical history and comfort goals.
Sedative medications act on the brain's anxiety pathways to lessen fear, blunt unpleasant sensations, and often shorten the subjective experience of time. For many patients this reduces the emotional and physical barriers that make dental visits difficult, allowing them to tolerate longer or more complex appointments. The calming effect can be especially helpful for people who have avoided care and now face restorative needs.
By reducing anxiety, sedation helps patients stay relaxed and cooperative so clinicians can work more efficiently and with fewer interruptions. That improved cooperation often permits combining procedures into fewer visits when clinically appropriate. Over time, successful sedated visits can break cycles of avoidance and support better long-term oral health.
Candidates include people with pronounced dental fear, those facing long or complex procedures, patients with a strong gag reflex, and individuals who have difficulty remaining still because of physical or cognitive limitations. Children with severe behavioral challenges may also be considered for specific sedation approaches when necessary and appropriate. Each case is evaluated on its own merits to determine the safest, most effective option.
A thorough review of medical history, current medications, and previous experiences with anesthesia is part of the candidate evaluation. The dental team discusses risks, benefits, and alternatives so the patient or caregiver can make an informed decision. If office-based sedation is not suitable, the team will recommend referral for hospital-based anesthesia when clinically indicated.
Common office-based options include inhalation sedation with nitrous oxide, oral sedation using prescribed medications, and intravenous (IV) sedation for more controlled effects. Nitrous oxide provides quick, adjustable relief and wears off rapidly after the gas is stopped. Oral sedatives produce a deeper sense of calm and drowsiness, while IV sedation allows rapid onset and easy adjustment during treatment.
The choice of method depends on the patient's health history, the length and complexity of the procedure, and the comfort goals discussed during consultation. All methods used in the office are administered by trained clinicians with appropriate monitoring in place. Preparation and recovery expectations vary by method, so patients receive clear instructions tailored to the chosen approach.
Conscious sedation produces a relaxed, semi-awake state in which patients can often respond to simple commands and breathe independently. This level of sedation is sufficient for many dental procedures performed in an office and typically allows faster recovery than general anesthesia. Conscious techniques prioritize maintaining airway reflexes and spontaneous breathing while reducing anxiety and discomfort.
General anesthesia produces a deeper, fully unconscious state and is generally reserved for situations that cannot be safely or effectively managed in the office setting. It requires administration and monitoring in a hospital or surgical center by an anesthesiologist. The dental team will recommend general anesthesia only when medical or procedural factors make it the safer option.
Preparation depends on the type of sedation selected but commonly includes fasting for a prescribed period, temporarily adjusting certain medications when advised, and arranging for a responsible adult to escort you to and from the visit. It is important to share a complete list of current prescriptions, over-the-counter medicines, and medical conditions before the appointment. Follow the pre-visit checklist provided so the care team can minimize risk and tailor monitoring to your needs.
On the day of treatment wear comfortable, loose clothing and avoid strong perfumes or heavy makeup that could interfere with monitoring equipment. Because some sedatives impair coordination and judgment, plan to rest for the remainder of the day and avoid driving or operating machinery until fully cleared by the team. If you have specific health concerns, discuss them in advance so the team at Dentistry of Sugar Land can customize your instructions.
During sedated care clinicians use continuous monitoring of vital signs such as oxygen saturation, heart rate, and blood pressure to track the patient's status throughout the appointment. Depending on the level of sedation, additional monitoring like EKG or capnography may be employed to ensure airway and cardiovascular stability. Trained staff are present to adjust medication levels and respond promptly to any changes.
Practices that offer sedation maintain emergency protocols and equipment, and clinicians receive training in airway management and resuscitation. Dosing is individualized based on medical history and real-time response, and communication with the patient remains a priority when conscious techniques are used. Clear post-procedure observation is provided until the patient meets discharge criteria and is safely handed off to a responsible escort.
Recovery varies by the sedation method used: nitrous oxide wears off quickly and patients often feel alert within minutes, while oral and IV sedatives require more time for effects to diminish. Patients are typically observed in the office until vital signs are stable and then discharged to the care of the escort they brought. Rest for the remainder of the day is recommended, and normal activities can be resumed when the team gives clearance.
During recovery avoid alcohol, driving, and operating heavy machinery for the period advised by your clinician because sedatives can impair judgment and coordination. Follow any written aftercare instructions provided, including restrictions on eating, drinking, and medication timing. Contact the office promptly if you experience unexpected symptoms such as prolonged dizziness, difficulty breathing, or severe bleeding.
Some sedatives, particularly certain oral and IV medications, can produce partial or complete anterograde amnesia so patients have limited recall of the procedure. Nitrous oxide generally has minimal impact on memory and is more likely to allow patients to remember parts of the visit. The degree of memory impairment is related to the type and depth of sedation used and is discussed during the informed-consent process.
Limited memory can be an intended and beneficial effect for patients who find the thought of dental treatment distressing. The care team explains what to expect beforehand so patients and caregivers understand how the medication may affect recollection and recovery. If memory or cognitive effects are a concern, the team will recommend an approach that balances comfort with your preferences for awareness and recall.
Determining whether sedation is appropriate begins with a consultation in which the dental team reviews your medical history, discusses your anxiety and treatment needs, and explains the available options and safety measures. Together you will weigh the potential benefits and limitations of each sedation method and consider alternatives such as behavioral techniques or short, staged appointments. The goal is a personalized plan that supports your health and comfort while minimizing risk.
When office-based sedation is recommended, the team outlines pre-visit instructions, monitoring protocols, and recovery expectations so you know what to expect. If a higher level of anesthesia is indicated for medical or procedural reasons, the practice will coordinate care with the appropriate facility and specialists. To learn more or to schedule a consultation, contact Dentistry of Sugar Land and the team will guide you through the next steps.
Ready to schedule your next dental appointment or have questions about our services?
Contacting Dentistry of Sugar Land is easy! Our friendly staff is available to assist you with scheduling appointments, answering inquiries about treatment options, and addressing any concerns you may have. Whether you prefer to give us a call, send us an email, or fill out our convenient online contact form, we're here to help. Don't wait to take the first step towards achieving the smile of your dreams – reach out to us today and discover the difference personalized dental care can make.